Current Research Projects:
Optimizing surgical treatment of crouch gait on a patient-specific basis
Crouch gait is a prevalent and troublesome characteristic of patients with cerebral palsy. The knee does not fully extend during gait which impedes function and puts these patients at risk of patellar stress fractures. The severity of the flexion contracture can worsen over time, and surgical intervention is often required for these patients. This project focuses on developing a comprehensive platform for evaluation of surgical treatment of crouch gait on a patient-specific basis. A combination of experimental and computational methods are used, including 3D patient kinematics, rigid-body musculoskeletal modeling, and finite element modeling of the lower limb and knee joint, to develop in-depth understanding of joint mechanics and motions of patients with crouch gait. This is used to simulation surgical options which will aid the clinician in determining which treatment pathway best restores normal quadriceps efficiency, while minimizing stress in the patellar cartilage and strain in the underlying patellar bone. This project is in collaboration with Children’s Hospital, Colorado, and is funded through the Mountain West Clinical Translational Research – Infrastructure Network (MW CTR-IN) subaward number 17-756Q-BSU-PG67-00 under a grant from National Institute of General Medical Sciences NIGMS of the National Institutes of Health under award number 4U54GM104944.
Evaluation and treatment of recurrent patellar dislocation
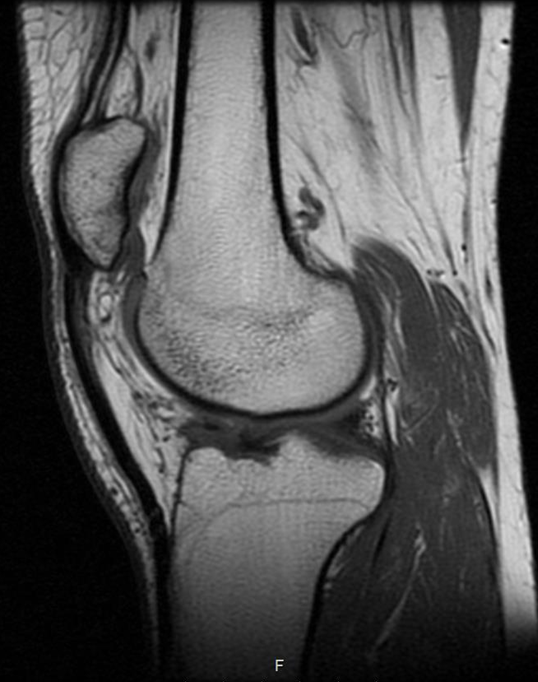
Patellar dislocation is a debilitating injury which typically occurs during sports-related activities in young active people. Patellar dislocation accounts for 2-3% of all knee injuries, and over 20,000 people per year, primarily in their teenage years, are affected by an initial incidence of patellar dislocation. After initial dislocation, the incidence of reoccurrence is almost 50%. There is little consensus on the treatment of patellar dislocation, which varies from conservative management through physical therapy to surgical interventions including medial patellofemoral ligament (MPFL) reconstruction, tibial tubercle osteotomy and sulcus-deepening trochleoplasty. This project incorporates a combination of in-vivo patient imaging with state-of-the-art musculoskeletal and finite element modeling. Subject-specific musculoskeletal models are developed for a cohort of patients with recurrent patellar dislocation and control subjects. Validated models predict muscle loading and patellofemoral mechanics during dynamic activity on a subject-specific basis. This computational tool is applied to determine optimal treatment pathways on a patient-specific basis. This project is in collaboration with Mount Carmel Health System, Columbus, Ohio.