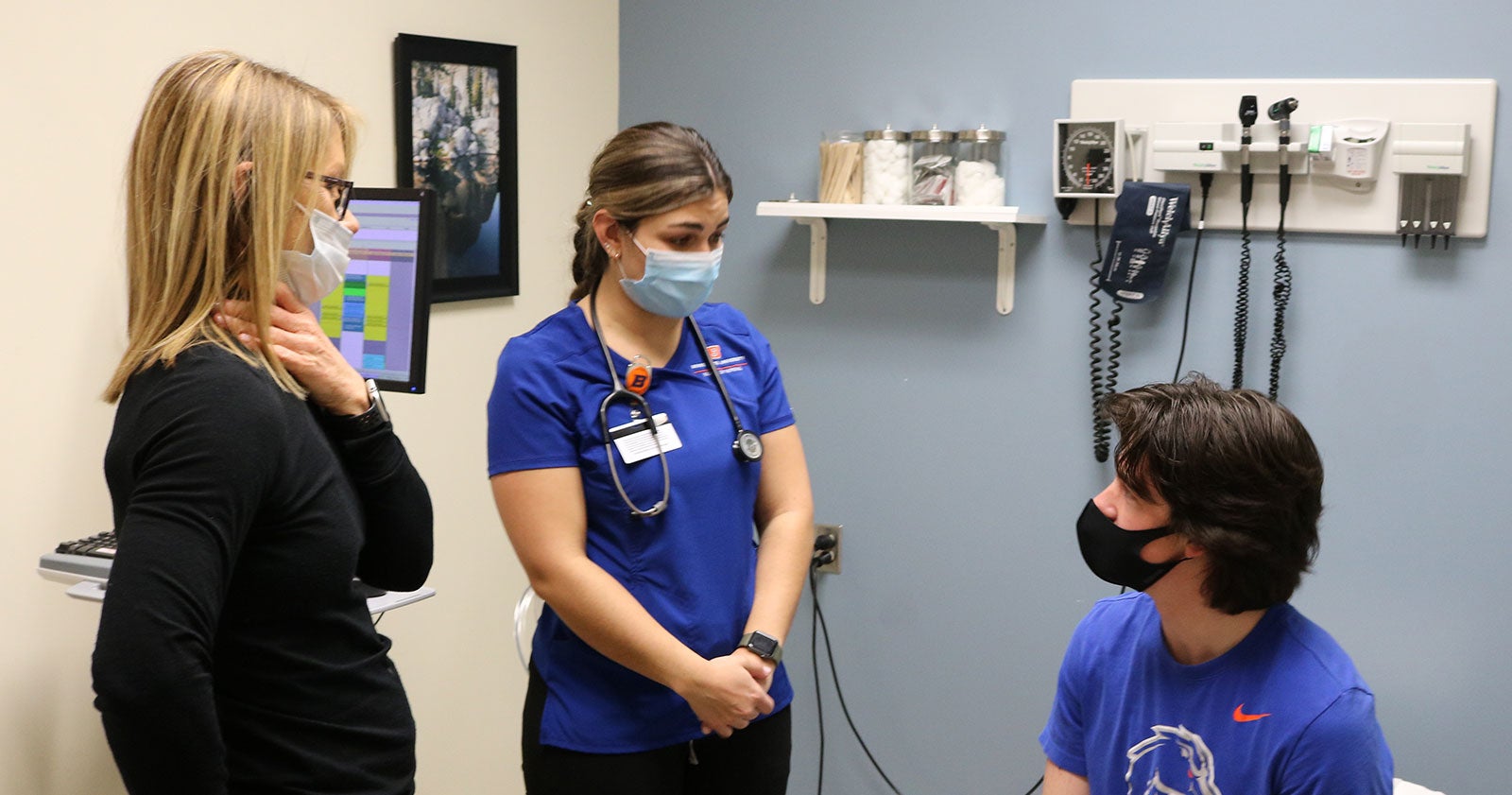
All good nurses get better with practice.
And Boise State, the College of Health Sciences, the School of Nursing – and now, University Health Services – are making sure baccalaureate registered nursing students get all the practice they need to go out into the world with the confidence to be great at their jobs.
The university, college and school partner with multiple hospitals and health systems for valuable clinical exposure and experience and have for years. The challenge has been to keep up with those needed practical hours during the pandemic, when hospitals and health systems have faced their own challenges with COVID-19, patient counts and staffing levels. School of Nursing faculty members themselves have needed to get creative to ensure that students receive direct patient care experience in addition to high-fidelity simulation and lab experiences.
Enter Stacey Hanrahan, a School of Nursing clinical assistant professor and nurse practitioner who works per diem in University Health Services. Wearing her various hats, she could see the bottleneck – and an innovative solution.
“I was thinking, ‘We have got to find some alternative clinical opportunities for these students,’” she recalled. “It’s created a challenge.”
Boise State’s registered nurse students routinely rotate through a variety of experiences in the hospital setting, including exposure to various specialties such as endoscopy and medical imaging, pharmacy and medical/surgical functions. To be eligible for licensure, students need dozens of hours.
In recent weeks, many of the school’s registered nurse students agreed to participate in clinical opportunities within University Health Services, allowing them to get needed hours and experience nursing functions outside the hospital setting.

A new student clinical experience
Under the supervision of their instructor, a registered nurse, and partnering with the licensed professional clinicians of the University Health Services team, they’ve welcomed patients while walking them to exam rooms– many of whom are fellow Broncos, but also faculty members and employees – taken patient vitals (blood pressure, height, and weight), given allergy injections and immunizations, completed medication refills, done phlebotomy – blood draws – and conducted phone follow-up, along with other functions.
Natalie Cacchillo, from Boise, has been one of those students. As with the others, she is in her fifth of eight semesters for the registered nurse bachelor’s program; unlike others, she works at Saint Alphonsus now as a nurse apprentice, with a goal of becoming a nurse practitioner, possibly in family or internal medicine.
Her time with University Health Services was productive – and very busy.
“I got to do throat swabs, I got to do flu swabs, I got to do mono spot tests, I got to draw blood, I got to give allergy injections,” she said. “It’s very different. I think it’s great. It’s really good experience.”
Both the range of care offered through University Health Services and by the staff impressed her.
“A lot of the nurses wanted to help me learn,” she said.
The feeling was mutual.
“They have done a really great job, as has my staff really welcoming these guys. They are seeing everybody from across campus,” said Julia Beard, University Health Services executive director. “It’s very different than the hospital. I’m an RN, and the thing that’s always true about being an RN is you just never quite know what’s going to happen next.
“This is an example of how these students can go on to do a lot of different things. It’s a really great experience for them.”
The exposure, quite literally, is broadening.
“It gives the students the opportunity to see other roles nurses have outside the acute care setting,” Hanrahan said.

Cacchillo echoed that observation – and saw the silver lining in the change of plans.
“My favorite part was that it’s a less acute setting,” she said. “You get to spend more time with your patient.”
A wide world of nursing
The placement design has been a necessary innovation, but because so much of nursing happens outside of hospitals – in schools, in the community, internal medicine, family medicine, in ambulatory care settings – the experience is likely to be what real life for some of these soon-to-graduate students is like.
It’s a first among these parts of the university, Hanrahan believes, but may not be the last such collaboration.
“We have this resource,” she said. “We need to take advantage of it.”
Amy Spurlock’s a fan of the approach. Spurlock is the associate divisional dean and chief nursing administrator of the School of Nursing who has supported putting the pieces together to support the students. She gives the credit to Hanrahan and Beard.
“It was their great idea,” she said. “It’s wonderful when you have faculty and peers that are forward-thinking and solutions-based. It’s very easy to support good ideas.”
COVID-19 may have spurred the adjustment to the skills component of the training, but building out the option puts more tools in the toolkit for Boise State faculty members and students alike.
“During the pandemic, with healthcare organizations experiencing such a significant amount of change, and challenges due to the acuity and number of patients, it has resulted in us having to rethink some of those experiences,” Spurlock said.
Those taking part have seized the opportunity, Beard noted.
“The thing I’ve really enjoyed about them, and the staff as well, is that they’re very enthusiastic and very willing to jump in and do something that they have or haven’t done before,” she said. “They ended up in a completely different site, they’re doing urgent care, and so their ability to think on their feet and be nimble has really been great.”
Spurlock credits her colleagues – and students – for being nimble, given the circumstances.
“It’s required a lot of flexibility and creativity in planning these clinical experiences. It helps to have creative thinking, so this new partnership is a win-win.”
Spurlock sees the silver lining that Hanrahan does, given the nature –and future – of nursing.
“I completely 100% agree with her,” Spurlock said. “The models of care are changing, that traditional setting is changing.
“RNs are needed everywhere.”