Most of Boise State’s nurse practitioner studies occur online, but each year’s summer intensives present the opportunity to build hands-on skills, connect with faculty and peers, and learn through simulations.
Given the provider shortage and increasing need for mental health care, 2024’s students were offered more practice in mental health simulation and differential diagnoses than years past.
Director of Simulation-based Education and Research Tracee Chapman crafted two new simulation scenarios to do so.
Scenarios with real-world application
Differential diagnoses and avoiding assumptions
Chapman wrote one scenario that introduces students to a standardized patient who, on the surface, appears to be a textbook example of a repeat emergency room patient. But patient care is often more complicated.

“This scenario is aimed at differential diagnoses and identifying an opportunity to rescue a patient with a serious health condition,” Chapman said.
Chapman described differential diagnosis like a tree where providers “start with the branches” and “narrow down into the trunk.” Providers look at a patient’s presenting symptoms and, through diagnostic tests, seek to narrow them to the actual cause of the symptoms.
For example, if a patient presents with abdominal pain, providers think of what could cause it: appendicitis, heartburn, or maybe an ulcer. To narrow down their diagnosis, they use different diagnostic tests – like X-rays or CT scans – to land on an accurate diagnosis.
The goal of this simulation is for students to use differential diagnoses and identify that the patient’s medications are not being managed properly, Chapman said.
The scenario offers realistic, relevant practice for students since nurse practitioners specializing in acute care often work in emergency room settings.
“They have great potential of seeing patients who have unmanaged medications, unmonitored chronic conditions and emergent situations,” Chapman said. “We’re trying to combat the stereotypes that providers might run into and help students realize that patients present in all sorts of ways.”
Equipping students as a source of help and hope
In addition to her work in nursing education, Chapman also works with Canyon County as a certified emergency nurse and a board-certified sexual assault nurse examiner. So she wrote the second new scenario to equip students for interacting with victims of human trafficking.
While human trafficking is a difficult topic, Chapman emphasizes the importance of learning to identify opportunities to help individuals out of their circumstances.
“It happens all over the country, and we’re serving students all over the United States,” she said.
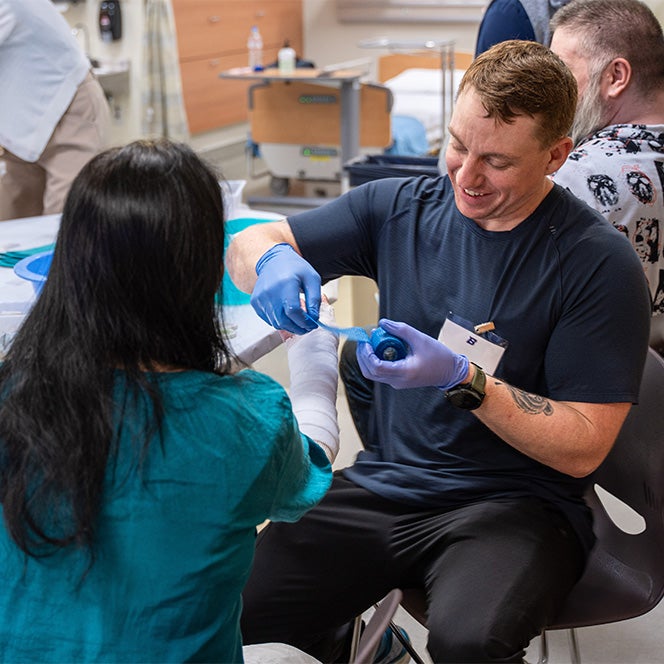
As with many simulations, the learning goals of this scenario are two-pronged: differential diagnoses and patient communication.
As a forensic nurse, Chapman said “it’s super important that we know how to talk to patients and not re-injure them.”
Students interact with standardized patients to practice wording questions that are trauma informed, offering resources and referring patients for help beyond their immediate health issues.
By increasing students’ education around interacting with this patient population, Chapman hopes “we can intervene, get them help and get them on to a better quality of life,” she said.
If you believe you are a victim of human trafficking or may have information about a potential trafficking situation, please contact the U.S. National Human Trafficking Hotline. The hotline also provides support and educational resources on their website.
A new approach for graduate students
The School of Nursing most often uses simulation with undergraduate students, but when Interim Divisional Dean Kelley Connor and program director Nicole Loos-Bartlett pitched new simulations for graduate students, Chapman made their ideas a reality.
Chapman herself is not a nurse practitioner, but as an expert simulation educator she was able to write scenarios alongside Associate Professor Molly Prengamen, who verified the nurse-practitioner details.
“It was really helpful to have a teammate in-house,” Chapman said. “I’m grateful for the opportunity to work across programs.”
Chapman designed the scenarios so that, for the first summer intensive session ever, graduate students used the same simulation structure of the pre-license scenarios. These include a full-class brief before the scenario; a small number of students participating in the simulation while the rest watch over video monitors; and a full-class debrief afterward.
Given the new scenarios, Chapman was excited for the nurse practitioner students to embrace this more traditional style of simulation.
“We know that whether you’re the student doing the activity or you’re the student observing the activity, it’s the debrief where the learning takes place and everyone learns the exact same information,” Chapman said. “That’s the beauty of simulation-based education.”