Prosthetic Socket Improvements
In this video, see how test prosthetic sockets are made. Closed captions and a video transcript are available.
One of the most common issues that lower leg amputees have is finding the perfect fit for their prosthetic leg. Due to the amputee’s activity and diet, the volume of an amputee’s residual limb fluctuates throughout the day that distorts the fit of their prosthetic socket which leads to discomfort, pain, and sometimes even serious medical complications. A new prosthetic socket design is required which has the capabilities of sensing a change in the user’s volume around the residual limb and actively provides action to fix the situation. Using new software, our team derived a solution to allow for a socket to accommodate for this fluctuation.
In this video, see how test prosthetic sockets are made. Closed captions and a video transcript are available.
Amputees typically see volume fluctuations in the residual limb throughout the day that affect the fit of their prosthetic socket which leads to discomfort, pain, or serious medical complications. A new design is required which has the capabilities of sensing a change in the user’s volume around the residual limb and actively providing action to fix the situation.

We determined the major concerns for stakeholders to be as follows:

To demonstrate the functionality of the pressure sensors and motors, we will first create a control system separate from the prosthetic. The purpose of this test is to test our control system. We will fine tune the coding to create a relationship between the applied pressure and the turning of the worm gear. We will directly measure the force inside the socket exerted on the residual limb using pressure resistors. An Arduino will receive the pressure input and control a worm geared motor that adjusts the tension of the tightening cable. Worm gearing is important to prevent any backsliding of the motor.
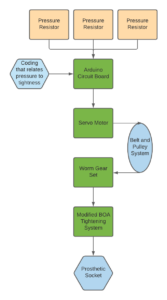
This design makes use of existing BOA socket tightening systems and automates the tightening process.
The design would utilize force sensing resistors located on the panel in contact with the tibia to measure the pressure on the limb. The tibia is one of three identified contact points with the existing socket. The data will be sent to an Arduino that would reside under the boa tensioner. The Arduino would interpret the data and drive a servo motor that would lead into a pulley system which drives a worm gear system to control the boa tensioner. The worm gear allows the system to be controlled in both directions to accommodate for increases or decreases in volume.
As per the list of specification, the user sees a pressure of around 20-60kPa in order to hold the socket to their residual limb. The sensor that has been selected has bounds from 0.646-151kPa. Being well within the range that the prosthetic will see and easy to adhere to the socket itself, these resistors will be an excellent choice for data collection.
The Arduino will be able to receive analogue input from the sensor and use it to make decisions controlling the motor.
The original Boa system uses a ratcheting mechanism to ensure it does not loosen during use. To achieve this same effect while also being able to tighten and loosen as necessary, a worm gear set will be used to provide one-way power transmission from the motor to the Boa. This will keep the load off of the motor when not actively tightening/loosening, as well as prevent “backsliding”. The motor selected provides 16kg-cm of torque while maintaining 12RPM.
The Boa tightening system has been provided by Kormylo – Advanced Prosthetics and Orthotics. This device has mapped out areas that have been determined as areas of contact critical for maintaining a tight fit with the patient. The Boa system is integrated into a prosthetic socket and will be modified in order to accommodate for the added electronics.
Our concept will need to be tested to ensure both safety and functionality of the socket. Testing goals and procedures are TBD, and may include any of the following: